Family Balancing/Gender Selection
NCCRM offers pre-implantation genetic diagnosis (PGD) and pre-implantation genetic screening (PGS) for the purpose of family balancing or sex selection by testing for the chromosome content of an embryo. Male embryos will have an X and Y chromosome, while female embryos will have two X chromosomes. This technology is also used to screen for additional chromosome abnormalities, to increase the chances of having a successful pregnancy and healthy baby. PGD is the most accurate known method for successfully determining sex prior to conception.
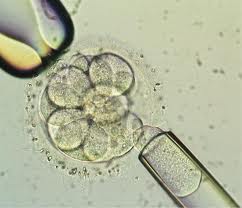
Do I need testing?
Pursuing IVF with genetic testing is a deeply personal and medical decision. Your IVF physicians can help you determine your likelihood of passing on a genetic disease and will steer you on the right path for your family. It is important to thoroughly discuss among yourselves and your physician what path is best for you.
How are embryos normally chosen?
In traditional IVF embryos are chosen based on their appearance, meaning your IVF physicians will determine which embryos should be transferred based on which look like the most likely to get you pregnant. However looks can sometimes be deceiving. An embryos genetic makeup is critically important in its development and for many couples, it is the deciding factor in whether you get pregnant or not. Embryos can contain specific genetic disorders, sometimes affecting the certain genes, and sometimes affecting entire chromosomes.
Avoid an inherited genetic disorder
Many patients go through IVF to avoid a specific genetic disorder affecting their family. Pre-Implantation Genetic Diagnosis (PGD) is a procedure designed to detect the genetic mutations which cause a specific genetic disorder in your embryos. The goal of PGD is for you to start day 1 of your pregnancy with the peace of mind that you’re building a healthy family. For families with certain blood disorders who have children with the disease, our PGD team can develop a test that will examine your embryos for both the specified genetic mutation but also for an HLA match for your sibling. Cord blood from an HLA match can be used to cure your existing child.
Screen for Chromosome Abnormalities
Some patients who have had recurrent spontaneous miscarriages, who have had recurrent losses even with IVF, who are of advanced maternal age, or who are at risk for male factor infertility elect to undergo chromosome screening.
Some imbalances come in the form of an abnormal number of chromosomes. An individual carries two copies of each chromosome, one copy from their mother, and another from their father. Sometimes, an embryo can carry an extra copy or be missing a particular chromosome(s) which in most cases leads to spontaneous miscarriage. Occasionally however a pregnancy that is chromosomally abnormal can be carried to term. The goal is to implant healthy embryos that have the highest chance of getting you pregnant due to their normal copy number of chromosomes.
Screen for Chromosome Translocations
Patients with a known chromosome translocation in their family elect to undergo chromosome screening to avoid getting pregnant with an embryo carrying an unbalanced version of the translocation.
Replacing Fewer Embryos
The goal of all our testing is to replace the fewest embryos possible that have the highest chance of getting you pregnant. By replacing fewer embryos, there is less chance of having multiples, and healthy embryos can be stored and implanted until you get pregnant.
To learn more or schedule a consultation:
Call (919) 233-1680 or


